Recognizing lymphedema early makes a significant difference in managing this chronic condition. It occurs when the lymphatic system fails to drain fluid properly.
leading to swelling that develops gradually and often goes unnoticed until it progresses.
What is Lymphedema
Lymphedema is a chronic disorder where excess lymph fluid collects in tissues, causing persistent swelling. Normally, lymph nodes and vessels circulate fluid, filter waste, and support immunity. When damaged or blocked, fluid accumulates, most often in arms or legs, though it can affect the chest, abdomen, or genitals.
Indications and Early Signs
The hallmark sign is swelling in one limb or body part, which may feel heavy, tight, or uncomfortable. Skin can appear shiny or stretched, and flexibility in nearby joints may decrease.
Early warnings include jewelry or clothing suddenly fitting tighter, or a feeling of fullness before visible swelling appears.
Progressive Indicators
As lymphedema advances, swelling persists despite elevation, movement becomes restricted, and skin texture changes. Over time, the skin may thicken, harden, or develop fibrosis.
Types and Causes
Lymphedema can develop for different reasons, depending on whether the lymphatic system is abnormal from birth or damaged later in life.
Understanding these distinctions helps explain why the condition appears at various stages and how different risk factors contribute to its onset.
- Primary lymphedema results from congenital abnormalities in lymphatic development. It can appear at birth, during puberty, or later in adulthood.
- Secondary lymphedema is more common, often caused by cancer treatments such as lymph node removal or radiation, as well as infections, injuries, or trauma.
Diagnosis
Doctors rely on physical exams, medical history, and limb measurements. Imaging tests like lymphoscintigraphy or MRI reveal blockages, while bioimpedance detects fluid buildup before swelling appears.
Differential diagnosis rules out other causes such as heart failure or kidney disease.
Stages of Lymphedema
- Stage 0: latent, no visible swelling but underlying damage.
- Stage 1: mild, reversible swelling responsive to elevation.
- Stage 2: persistent swelling with fibrosis, less responsive to treatment.
- Stage 3: severe enlargement, thickened skin, and major mobility limitations.
Signs and Symptoms
Persistent swelling is the most recognizable symptom of lymphedema, often worsening during the day and improving slightly with rest. Alongside swelling, individuals may experience physical effects such as heaviness, aching, and reduced joint flexibility, which can make movement tiring and uncomfortable. Skin changes are also common, with tightness, pitting edema, or a thick, leathery texture developing in more advanced stages.
Another concern is the increased risk of infection, particularly cellulitis, which presents with redness, warmth, tenderness, fever, and chills.
In severe cases, advanced lymphedema leads to significant enlargement of the affected limb, deep folds in the skin, warty growths, and restricted mobility, all of which can greatly impact daily life and independence.
Managing Symptoms
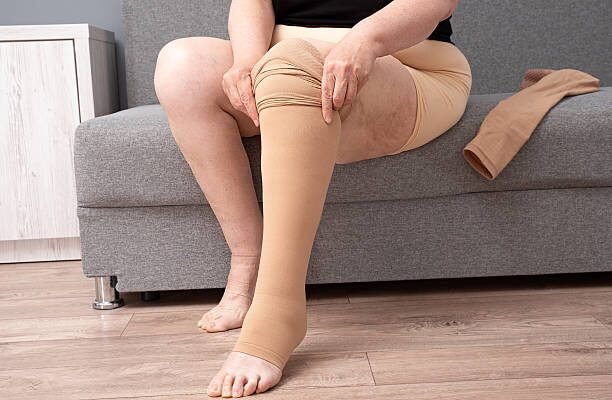
Treatment focuses on controlling swelling and preventing progression, often requiring both medical guidance and supportive care. Complete decongestive therapy combines manual lymphatic drainage, compression bandaging, exercise, and skin care.
Compression garments help maintain reduced swelling, while specialized massage and gentle exercise encourage fluid circulation. Proper skin care also reduces infection risk.
Seeking professional help through services like outcall massage can provide added convenience, allowing therapists to deliver lymphatic-focused treatments directly at home. This option supports those with mobility challenges and complements medical treatment plans, making symptom management more accessible and consistent.
Living with Lymphedema
Daily management involves adapting activities, using support groups, and following treatment plans consistently. With proper care, most people maintain active lives despite the chronic nature of the condition.
Risk Factors and Prevention
Several factors increase the likelihood of developing lymphedema, including cancer treatments that involve lymph node removal or radiation, obesity, and infections that compromise the lymphatic system. Preventive strategies focus on maintaining a healthy weight, protecting the skin from injury, and monitoring for early signs of swelling.
Individuals who have undergone cancer treatment should take extra precautions, such as avoiding blood pressure checks, injections, or blood draws in the affected limb, and protecting the skin from cuts or insect bites. Exercises like swimming or walking help promote circulation and reduce fluid buildup, while good skin hygiene and protective measures further reduce infection risk.
Finding Professional Help
- When lymphedema symptoms suddenly worsen, it can be unsettling, especially if you’re away from your usual healthcare providers and relying on local wellness options.
- Seeking professional care is essential in these moments.
- Immediate medical attention is needed for rapid swelling, particularly after cancer treatment, or if signs of infection appear such as redness, warmth, fever, or chills.
Alongside medical care, supportive therapies can help manage discomfort and improve mobility. Specialized clinics and wellness centers in popular tourism areas often provide treatments designed to support recovery and overall wellness, including lymphatic drainage massage in Bali, which focuses on gently moving fluid and reducing swelling.
Conclusion
Lymphedema is a chronic but manageable condition. Recognizing early signs such as heaviness, tightness, or subtle swelling allows timely treatment. With consistent management, including therapy, compression, exercise, and skin care, most individuals maintain quality of life. While incurable, lymphedema can be controlled through proactive care and medical support.

