Amy Lightner, MD, is a physician-scientist and colorectal surgeon whose work bridges clinical care and research in inflammatory bowel disease. Based in CA, she serves as a Professor at the Scripps Research Institute and practices with the Scripps Clinic Medical Group. Her expertise spans immunology, microbiology, and translational medicine, with a focus on developing innovative therapies for conditions such as Crohn’s disease and ulcerative colitis. Dr. Amy Lightner has led clinical trials, directed major regenerative medicine centers, and contributed extensively to scientific literature, making her a leading voice in understanding the risks and complications associated with inflammatory bowel disease and advancing patient care.
Understanding Risks and Complications of Inflammatory Bowel Disease
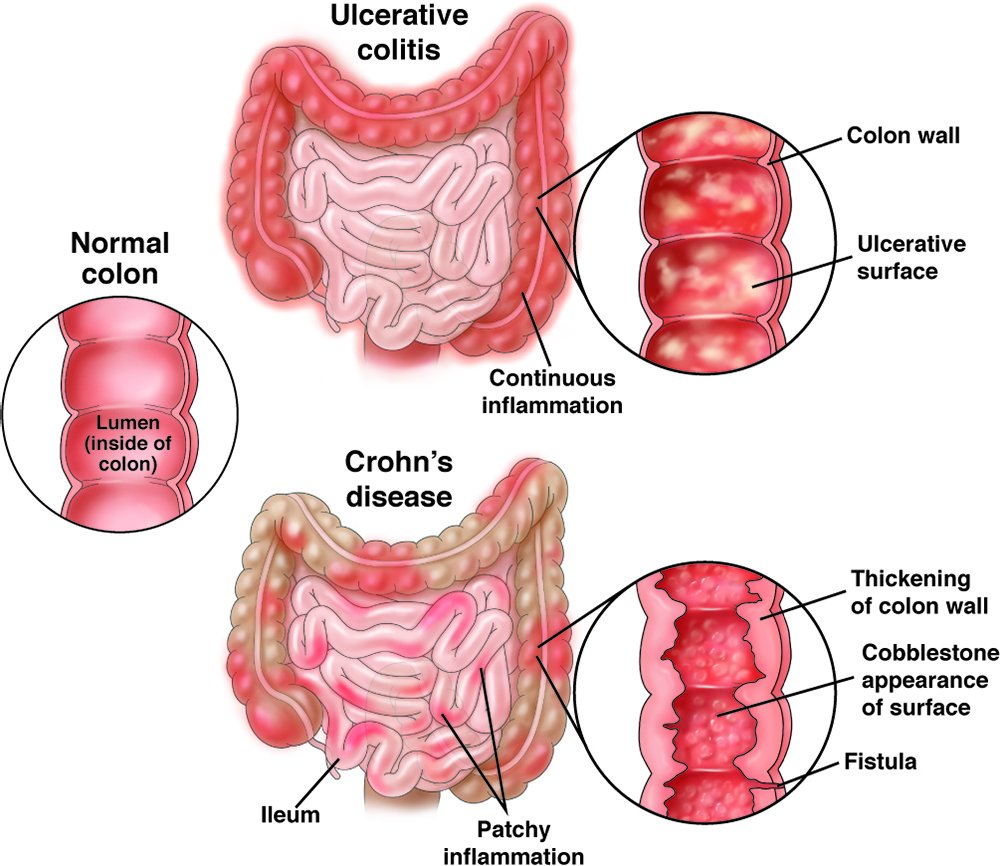
Inflammatory bowel disease (IBD) ranks among the most common health conditions in the United States. According to the Centers for Disease Control and Prevention, IBD prevalence in the country ranges from 2.4 million to 3.1 million people in 2024. Furthermore, prevalence has risen in recent years, driving health care costs toward $9 billion annually. To develop more impactful, long-term treatments for IBD, both medical professionals and average Americans must develop a more comprehensive understanding of the disease.
To start, IBD is not a single health condition but rather an umbrella term that describes several conditions defined by swelling and inflammation of digestive tract tissue. One common examples of IBD is ulcerative colitis, a condition characterized by inflammatory sores, called ulcers, that form throughout the colon and rectum. Another, Crohn’s disease, can cause severe, debilitating pain due to inflammation of the intestines, bowels, and upper gastrointestinal tract.
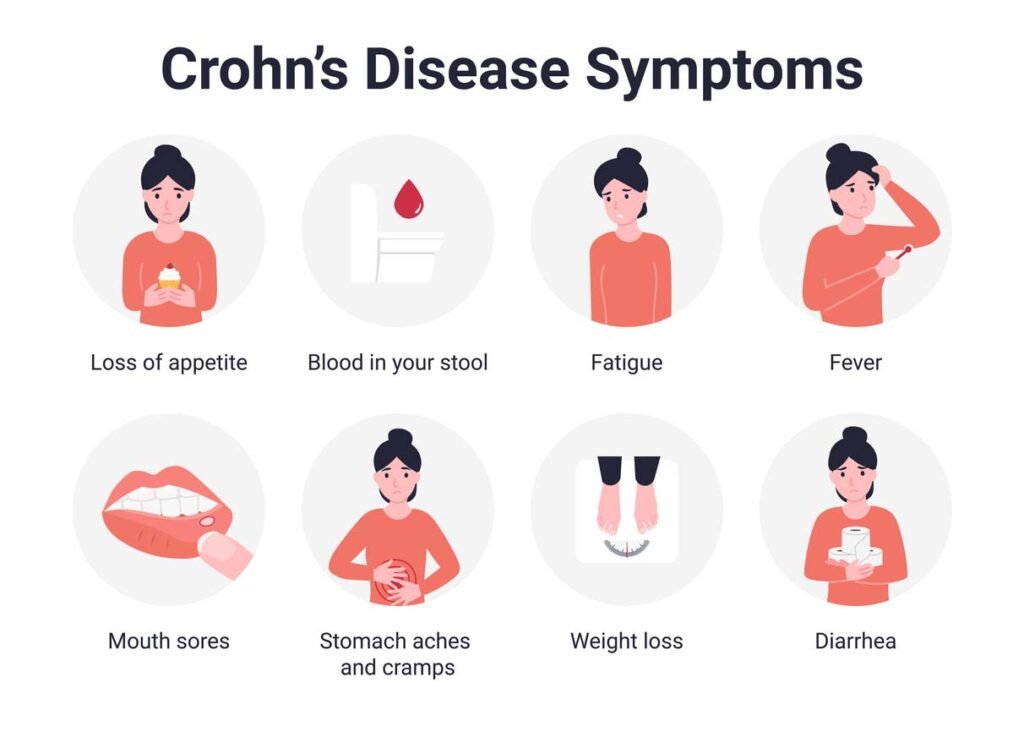
Americans may struggle to identify early signs of IBD. Diarrhea and belly cramping, for example, rank among the most common health issues in the United States and can occur for many reasons, most of them minor and temporary. Other basic symptoms range from fatigue to a loss of appetite. If these symptoms persist, or if they are accompanied by unexplained weight loss and bloody stool, individuals should consult with a medical professional.
Americans should exercise particular caution if they live with an increased risk of IBD. Individuals who have experienced immune system complications, for instance, may have issues with their body attacking cells in the digestive tract, causing inflammation and IBD complications. Risk can increase with factors such as growing up in a sterile environment that minimizes germ exposure or taking antibiotics early in life. Genetic factors also likely play a role in IBD development, though doctors are unclear on the specifics, and many people living with IBD have no family history of the disease.
Many additional uncontrolled and controllable risk factors can influence a person’s likelihood of developing IBD. Unlike many chronic diseases, the older a person gets, the lower their odds of an IBD diagnosis; most individuals develop IBD before the age of 30, though a diagnosis over the age of 50 or 60 is not impossible.
While people of all ethnicities have demonstrated the ability to experience IBD symptoms, the disease most commonly impacts white people. Family history is another uncontrollable factor; while doctors and researchers do not believe IBD results from inherited genetic traits, people who have blood relatives with IBD are more likely to develop the disease themselves.
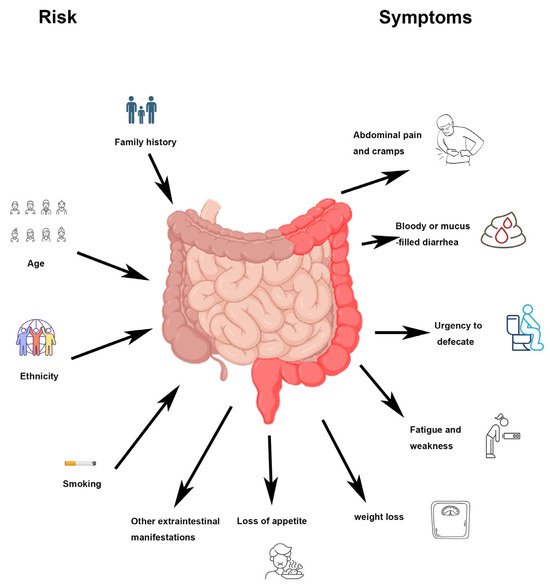
When it comes to controllable risk factors, individuals should refrain from cigarette smoking, which greatly increases a person’s risk for many health conditions, including Crohn’s disease. Excessive use of Advil, Aleve, and other nonsteroidal anti-inflammatory medicines can also influence a person’s risk profile.
Understanding these influencing factors is paramount to a person’s health. While some IBD symptoms may qualify as mild inconveniences, if left untreated, the disease can lead to major, life-threatening health complications, including an increased risk for colon cancer. IBD symptoms can also lead to liver damage, fatal blood clots, malnutrition, and severe dehydration, as well as complications such as toxic megacolon and colon perforation. With a clearer understanding of IBD’s risks and complications, Americans can assume greater responsibility for their bowel health and overall wellness.
About Amy Lightner
Amy Lightner, MD, is a physician-scientist and colorectal surgeon at Scripps Clinic and a Professor at the Scripps Research Institute. Her work focuses on inflammatory bowel disease, combining clinical care with translational research in immunology and regenerative medicine. She has led major programs at the Mayo Clinic and Cleveland Clinic, conducted clinical trials, and published extensively. Dr. Amy Lightner also serves in editorial roles for leading journals and has received multiple research grants and awards.
Research based Reference:
- https://www.cdc.gov/ibd/data-statistics.htm
- https://pubmed.ncbi.nlm.nih.gov/30694325/
- https://www.sciencedirect.com/science/article/pii/S0016508520304022
- https://www.nature.com/articles/s41575-020-00363-5
- https://academic.oup.com/ibdjournal/article/27/10/1559/6156736
- https://www.thelancet.com/journals/langas/article/PIIS2468-1253(19)30333-4/fulltext
- https://www.gastrojournal.org/article/S0016-5085(20)34737-5/fulltext

